Great Catches:
A “great catch” is when someone proactively prevents harm from reaching the patient. Great catches are celebrated each day at campus Daily Safety Briefings. Each month, Kettering Health selects a Great Catch of the Month, with a yearly winner selected and celebrated at the annual Quality Banquet.
Please share your great catches with your leader so your commitment to patient safety can be celebrated.
December 2021 Great Catch of the Month:
- Kalyn Patrick from Soin Medical Center noticed when a surgery patient arrived in Pre/Post-Op (PPO) from the ED that the patient’s armband was blank, and she was quick to place an appropriate armband on the patient. Thank you, Kalyn, for using two patient ID’s and noticing the armband was incorrect.
- Jenita Weathington, a transporter from Kettering Health Hamilton noticed a patient’s oxygen tank was on red and it wasn’t safe to use. She got a new tank with enough oxygen and possibly prevented a Serious Reportable Event (SRE).
- Erika Stevens an operating room nurse from Kettering Health Washington Township noticed that the surgeon did not see or mark the patient prior to surgery. Erika found the surgeon and ensured they saw and marked the patient appropriately. Thank you, Erika, for speaking up for safety.
Key Projects and goals for 2022
A Serious Reportable Event (SRE) is when a patient experiences death or serious harm due to an error or deviation from standard care practice. With the Kettering Health Zero Harm initiative, we are committed to reducing patient harm.
2022 SRE Goal
| 2021 Baseline | 0.51/1000 patient days |
| 2022 Threshold | 0.46/1000 patient days |
| 2022 Target | 0.41/1000 patient days |
| 2022 Stretch | 0.38/1000 patient days |
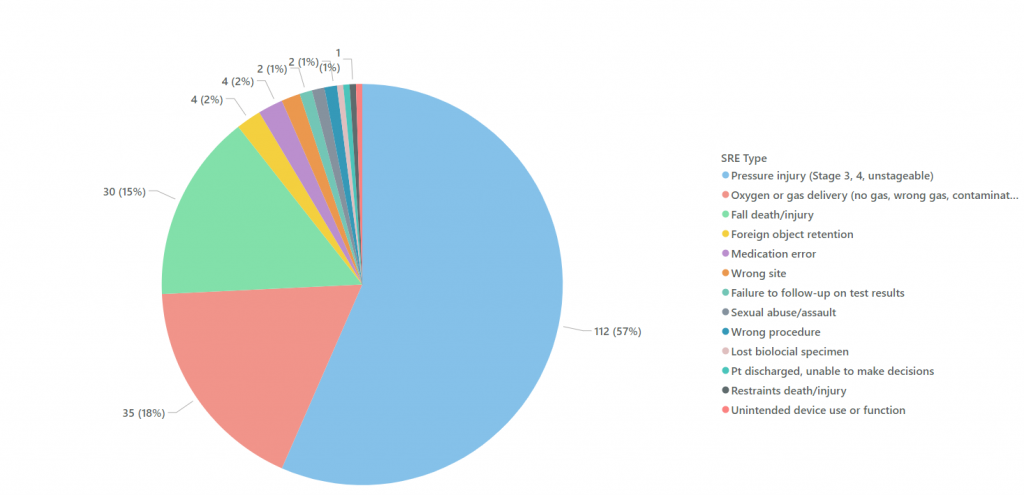
The pie chart below shows Kettering Health SRE’s for 2021. The largest area for improvement is reducing falls with injury, oxygen or gas delivery events (O2 events), and hospital-acquired pressure injuries (HAPI). 90% of the SRE’s in 2021 were due to falls with injury (15%), O2 events (18%), or HAPI (57%).
O2 Events Tanks:
- Kettering Health purchased new oxygen tanks that measure volume and time instead of pressure.
- The new tanks display how much oxygen is left in the tank in time.
- When there is a ¼ of a tank or 15 minutes left, the tank alarms.
- The tank alarms again when it is empty.
- The “Ticket to Ride” form has been changed to match the new tanks.
Implementation:
- The new tanks are in use at Kettering Health Main Campus and Washington Township.
- New tanks will be distributed to other Kettering Health facilities by the end of February 2022.
- Be on the lookout for a required HealthStream video that demonstrates how to use the new tanks and the best practice for a two-person hand-off with the “Ticket to Ride” during transport.
HAPI:
- HAPI present the greatest opportunity to reduce SRE for our system. An SRE HAPI is a hospital-acquired pressure injury that is a stage 3, stage 4, or unstageable.
- An analysis was performed on all SRE HAPI in 2021, and the root causes were grouped and key priority areas for improvement were identified based on the most common root causes of HAPI.
- It is important that a thorough assessment for wounds is conducted and documented on admission or transfer to the unit, or anytime the patient has been off the unit greater than two hours.
- Be on the lookout for an upcoming Safety Spotlight at Unit Huddles discussing key ways in which you can help reduce HAPI.
Medication safety:
This month’s focus is on Midas medication events reported due to extra doses being administered or medication being administered off schedule.
- There are Midas events reported when a medication is administered and documented as given on the MAR and then a few hours later, another dose is being administered of the same medication even though it was not due or not scheduled to be administered.
- Let’s review an example: Clopidogrel 75mg po daily at 9 a.m. and dose is administered and documented:
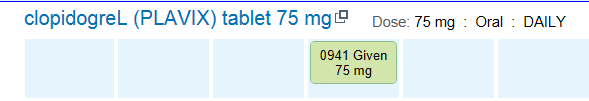
- Then six hours later, another dose is prepared to be administered.
- Epic alert appears that the dose has already been administered and is not due or scheduled to be given:
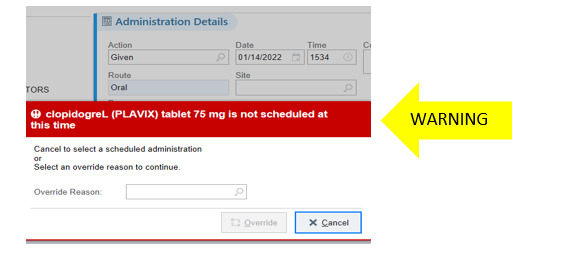
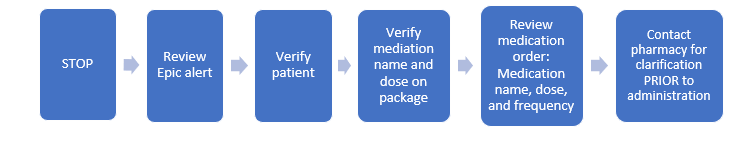
- In the above example: Epic requires an “override reason” for why medication is being administered even though it is not scheduled to be administered per the active medication order.
When the end user selects an override reason and continues with the administration, there needs to be a clinical reason and a provider order to administer a medication that was not scheduled to be or was already given.
When Epic alerts appear: